| ENTITY |
CONNECTIONS |
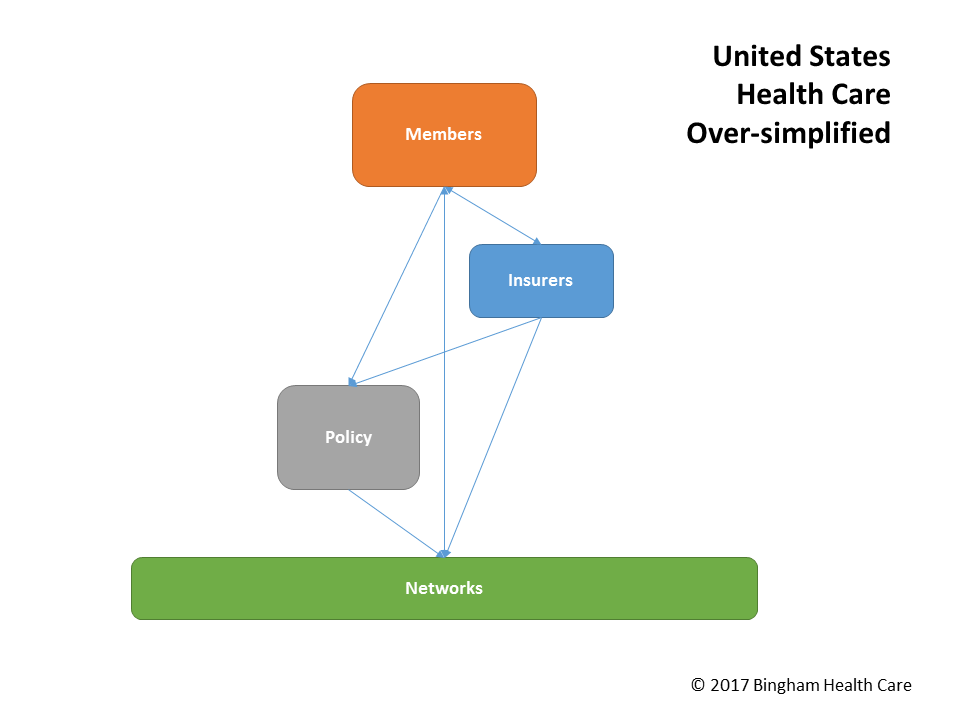
| MEMBER |
- purchases coverage from INSURER and pays monthly premiums to INSURER
- works with INSURER's member services, case managers, and authorization unit
|
- purchases a health care or health insurance POLICY that provides the member healthcare coverage
|
- visits / works with healthcare providers in the NETWORK to get health care benefits (services & products) per the policy's terms, conditions, & restrictions
- pays providers in the NETWORK deductibles, co-payments (co-pays), and co-insurance for provided health care services and products
|
| INSURER |
- sells coverage to MEMBER, bills MEMBER for monthly premium, and processes premium payments
- works with MEMBER to authorize care and to help resolve disputes with providers, and renew/retain coverage
|
- creates a healthcare POLICY to be sold to consumers; this POLICY contains benefits and other factors related to receiving care
- working with actuaries, utilizing market data and consumer segmentation & competitor analysis, prices the POLICY based on richness (scope of benefits and network make-up) and expected utilization
|
- contracts with providers and provider NETWORKS, determining fee schedule/structure and quality-of-care requirements
- pays providers in the policy's NETWORK for health care provided to members on the policy
|
| POLICY |
- identifies in-NETWORK providers, and contains terms, conditions, and restrictions for utilizing NETWORK providers when obtaining health care services and products
- indicates member costs and insurer financial responsibility for obtaining varying types of care from specific NETWORK providers / provider types
|
| NETWORK |
- provides health care services and products to MEMBERS
- bills or collects payments from MEMBERS for a portion or all of the cost of care; these payments are deductibles, co-payments (co-pays), and/or co-insurance
|